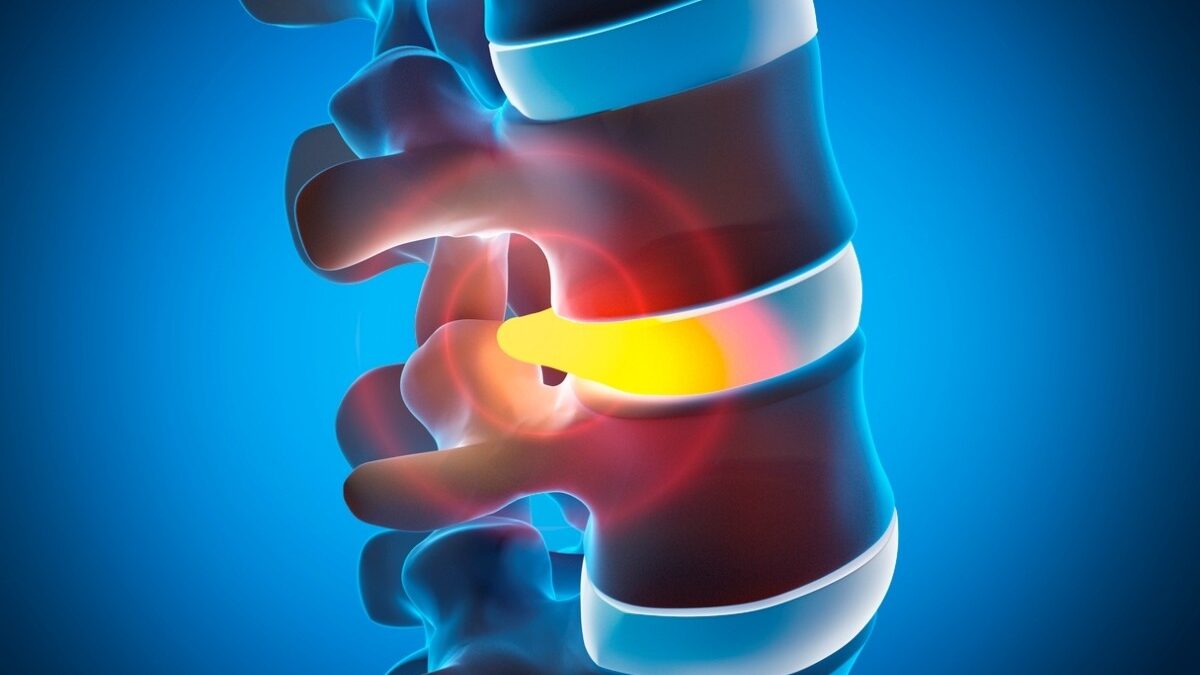
Slipped Disc Symptoms and When to See a Doctor
A slipped disc is one of the most commonly searched spine conditions, but the term can be misleading. Your spinal discs do not actually slip out of place. What most people are describing is a bulging or herniated disc. These discs sit between the bones of your spine, and each one has a tough outer layer and a softer center. A bulging disc occurs when the outer layer weakens and pushes outward. A herniated disc happens when the soft inner material pushes through a tear in that outer layer.
Either type can cause pain, especially when the affected disc puts pressure on a nearby nerve. Knowing what to look for can help you decide whether home care is enough or whether it is time for a professional evaluation.
How to recognize disc-related symptoms
Disc problems most often develop in the lower back and neck. The biggest indicator is the location of pain with nerve involvement. Pain that stays in one spot may not point to a disc, but pain that travels into an arm or leg is a much stronger signal.
Common signs include pain radiating down one side of the body, often described as having a burning, electric, or shooting sensation. You may notice tingling or numbness in the hand, fingers, foot, or toes. Some people may feel weakness in a specific muscle group: they may have difficulty lifting the foot or gripping objects, for instance. Pain that worsens with sitting, bending, coughing, or sneezing is another hallmark.
With lumbar disc problems, people often describe sciatica, which is radiating pain that travels from the lower back into the buttock, thigh, and sometimes all the way to the foot.
How disc pain differs from a muscle strain
A muscle strain usually causes soreness that stays in one area and does not travel down the arm or leg in a specific pattern. You might feel stiff after resting and better after gentle movement. Muscle pain is often tender to the touch and improves steadily within the first couple of weeks after the injury.
A disc problem often causes pain that follows a pathway, like tingling in specific fingers or shooting pain down the back of your leg. Numbness, pins-and-needles sensations, or weakness may also be present. Sitting for long periods often feels worse than standing, and coughing or sneezing can trigger a sharp flare.
It is possible to have both nerve and muscle pain occur at once. A disc flare can trigger muscle spasm, and a strain can irritate nearby tissues enough to mimic deeper pain. If symptoms are not improving or the pain radiates, a professional evaluation can help sort things out.
When a slipped disc needs urgent attention
Most disc issues improve with conservative care, but certain symptoms should prompt you to seek medical attention right away:
- New loss of bowel or bladder control
- Numbness in the groin or saddle area
- Progressive leg weakness or trouble walking
- Severe pain following a major fall or accident
- Unexplained fever or chills along with back pain
These symptoms are uncommon, but they can point to a serious problem that requires immediate attention.
When to consider imaging or a spine evaluation
Many patients ask whether they need an MRI right away. Not always. Many acute episodes improve within a few weeks, and imaging is most helpful when the results would change the treatment plan.
An evaluation may be appropriate if pain lasts longer than two to four weeks without meaningful improvement, if symptoms keep returning and limit daily life, or if there is persistent radiating pain, numbness, or weakness. If you cannot sleep, work, or function normally because of pain, that is another reason to be seen.
A thorough spine evaluation includes a detailed history and physical exam, with your provider checking strength, reflexes, and sensation. X-rays can show alignment and arthritic changes, but an MRI is typically the most useful tool because it shows discs, nerves, and soft tissues in detail.
Treatment options for a slipped disc
Most slipped disc symptoms improve without surgery. The best outcomes often stem from a plan that reduces irritation, restores movement, and builds support around the spine.
Activity modification. Short-term rest can help during a flare, but prolonged inactivity often leads to stiffness and weakness. Most people do best with gentle movement while avoiding specific triggers like repeated bending, heavy lifting, or prolonged sitting.
Anti-inflammatory care. Anti-inflammatory medication may help reduce pain when appropriate for your health history. Heat or ice can also be useful depending on what feels best.
Physical therapy. Therapy focuses on core stability, posture, body mechanics, and controlled mobility. This approach helps calm a current flare and reduces the chance of future episodes.
Injections. If pain persists or nerve symptoms are limiting function, epidural steroid injections may be considered to reduce inflammation around the affected nerve.
Surgery. Surgery is typically reserved for cases where symptoms continue despite conservative care or when neurologic function is at risk. A common procedure is microdiscectomy, which removes the portion of the disc pressing on a nerve.
Getting ahead of disc pain before it worsens
If your symptoms are mild and there are no red flags, short-term self-care at home is a reasonable starting point. Stay gently active, avoid movements that trigger flares, and pay attention to how your symptoms change over one to two weeks.
If pain is getting worse, radiating pain is increasing, or your daily function is declining, that is a good time to move from self-management to a professional evaluation. The right approach depends on whether your symptoms suggest nerve involvement and whether your recovery is heading in the right direction.
If your back or neck pain is traveling into an arm or leg, or if symptoms are not improving with at-home care, schedule an evaluation with Florida Surgery Consultants to confirm the cause and discuss the best treatment options for lasting relief.