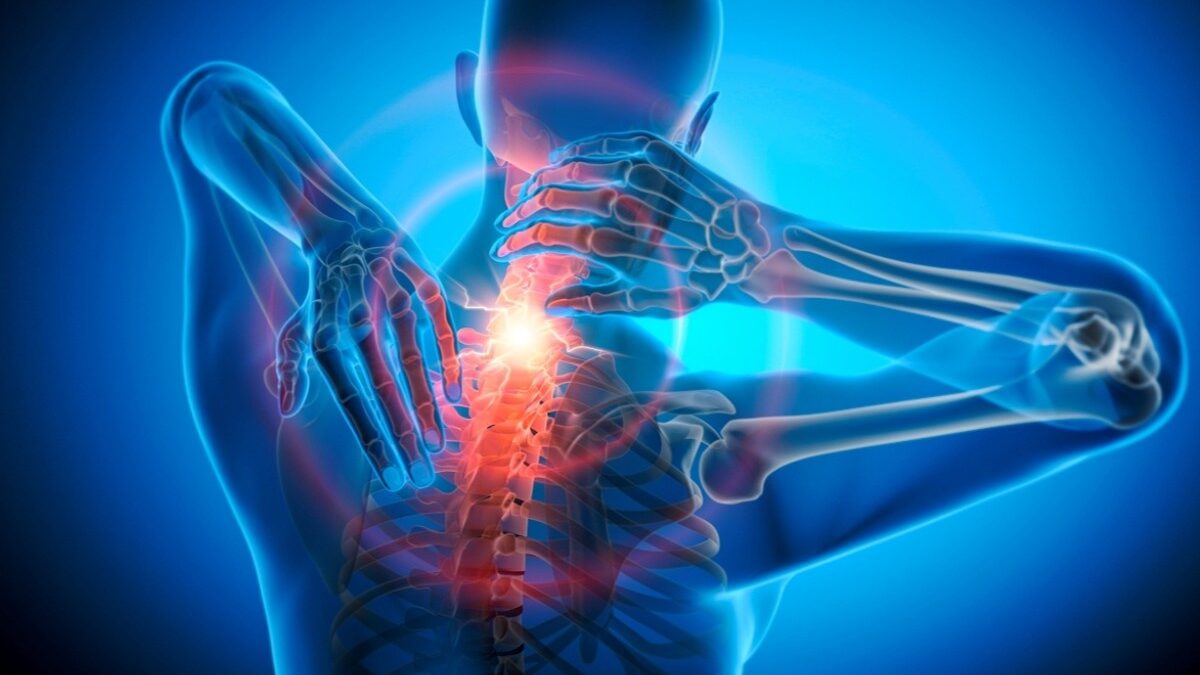
Foraminal stenosis is a narrowing of the small openings on each side of the spine where nerves exit. These openings are called foramina, and you have them at every level of the vertebrae from the neck through the lower back. When the space around a nerve root becomes too tight, the nerve can become irritated or compressed. This is one of the most common structural reasons people develop what is often called a “pinched nerve.”
The narrowing usually develops gradually from age-related changes in the spine, though it can also happen more suddenly after an injury. Many people with foraminal stenosis improve with conservative care, but if symptoms persist, minimally invasive procedures can help relieve pressure on the nerve.
What causes the foramen to narrow?
Several structural changes can reduce the space available for a nerve root. Degenerative disc changes are one of the most common contributors. As discs age, they lose height and hydration, which makes the foramen smaller and leaves less room for the nerve.
Arthritis in the facet joints can lead to bony overgrowth, often called bone spurs, which crowd the foramen. A bulging or herniated disc can also press into the opening, especially if it shifts toward one side. Over time, supportive ligaments and tissues around the spine can thicken and contribute to narrowing as well. Alignment or stability changes may also play a role and are evaluated on a case-by-case basis.
How to recognize foraminal stenosis symptoms
Symptoms depend on which nerve is affected and how much compression is present. Depending on the severity of the situation, some people notice symptoms that come and go, while others deal with constant discomfort that limits activity.
The hallmark of foraminal stenosis is pain that travels beyond the spine. In the neck, this may mean pain radiating into the shoulder, arm, or hand. In the lower back, it may mean pain traveling into the buttock, thigh, calf, or foot — a pattern often associated with sciatica. You may also feel tingling or numbness in the fingers, hand, toes, or foot, or notice weakness in a specific muscle group that causes difficulty gripping, lifting the foot, or climbing stairs.
Certain positions tend to make symptoms worse, such as looking up, twisting, or sitting or standing for long periods of time. Changing posture, resting, or leaning forward may bring temporary relief depending on the spinal level involved.
How is foraminal stenosis diagnosed?
A thorough diagnosis involves matching your symptoms, exam findings, and imaging results. Many people show narrowing on a scan without any symptoms at all, so the key question is whether the narrowing lines up with what you feel.
Your provider will ask where the pain travels, what triggers it, and whether you have numbness, tingling, or weakness. The physical exam typically includes strength testing, reflex checks, and sensation assessment to help identify which nerve root may be involved. X-rays can show alignment and arthritis, but an MRI is the most commonly used tool for evaluating discs, nerves, and foraminal narrowing in detail.
Conservative treatment options
Many patients improve without surgery. The goal of conservative care is to reduce nerve irritation, improve mobility, and strengthen the support system around the spine.
Short-term reduction of activities that reliably trigger symptoms can help calm the nerve, but this does not mean extended bed rest. Gentle movement and strategic pacing tend to support recovery better than complete inactivity. Anti-inflammatory medication may help when appropriate given your health history, and heat or ice can also provide relief.
Physical therapy is often a central part of treatment. For neck-related symptoms, therapy may focus on improving upper back and shoulder support. For low back symptoms, therapy often includes core stability, hip strength, and movement retraining. A good therapist can also teach you how to avoid positions that narrow the foramen and aggravate the nerve.
When injections or procedures may help
If conservative care does not provide enough relief, injections may be considered to reduce inflammation around the nerve root. Common options include epidural steroid injections and selective nerve root blocks. Some injections also help confirm the pain source by showing how symptoms respond when inflammation is reduced.
When foraminal stenosis continues to cause significant symptoms despite conservative treatment, or when weakness is present, a minimally invasive decompression procedure such as a foraminotomy may be recommended. The goal is to widen the space where the nerve exits by removing a small amount of bone or tissue that is crowding it.
When to seek urgent evaluation
Most foraminal stenosis symptoms can be evaluated in a standard office visit, but certain signs should be addressed promptly:
- Progressive weakness in the arm or leg
- Increasing numbness that is spreading or becoming constant
- Loss of coordination or difficulty walking
- New bowel or bladder control changes
- Severe pain after a fall or accident
These symptoms can indicate more significant nerve involvement that should not wait.
Protecting your spine and preventing flare-ups
Even after symptoms improve, addressing the factors that contribute to repeated irritation can help prevent setbacks. Many flare-ups are linked to posture strain, repetitive bending or twisting, prolonged sitting without breaks, or general deconditioning.
A sustainable long-term plan often includes consistent strength work for the core and supporting muscles, attention to ergonomics at work and in the car, and gradual progression of activity rather than sudden jumps in lifting or exercise intensity. The goal is not perfection. It is building enough resilience that the nerve is less likely to be irritated again.
If your pain is traveling, it is time to find out why
Foraminal stenosis can be confusing because symptoms often show up far from the spine itself. If you have pain that travels into an arm or leg, persistent tingling or numbness, or weakness that is affecting your daily movements, a focused evaluation can clarify whether a pinched nerve is involved and which level is responsible.
If your symptoms are persistent or getting worse despite conservative care, schedule an evaluation with Florida Surgery Consultants to confirm the cause and discuss your treatment options, including minimally invasive approaches when appropriate.