Back and neck pain can be caused by many different issues, but one of the most common culprits is a herniated disc. Also known as a slipped or ruptured disc, this condition can affect the spine’s ability to function properly and cause significant pain that radiates through the body. While the thought of spine surgery can be intimidating, the good news is that many herniated discs can be treated successfully without surgery.
What Is a Herniated Disc?
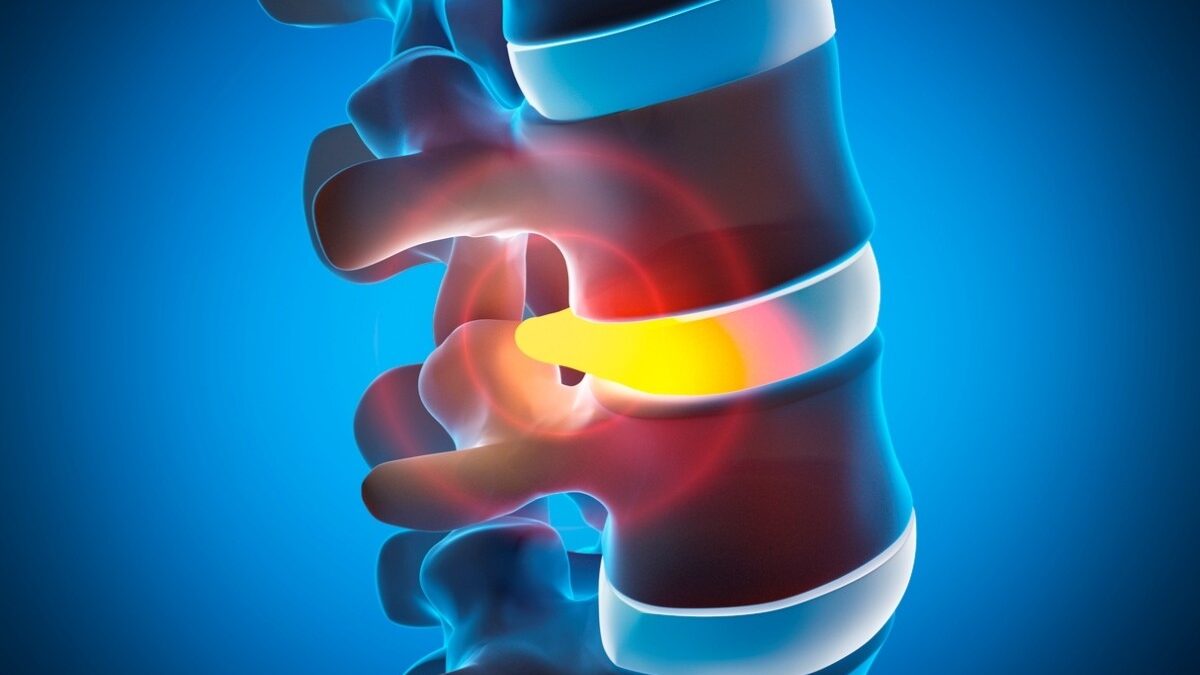
Your spine is made up of a series of bones (vertebrae) stacked on top of each other. Between each vertebra is a spinal disc: round, cushion-like structures that act as shock absorbers. Each disc has a tough outer layer and a soft, gel-like center.
A herniated disc occurs when the outer layer of the disc develops a tear or weak spot, allowing the inner gel to push through. This material can press on nearby spinal nerves, causing pain, numbness, or muscle weakness.
Herniated discs can happen anywhere along the spine, but they most often occur in the lower back (lumbar spine) or the neck (cervical spine).
What Causes a Herniated Disc?
Herniated discs can result from a sudden injury or develop gradually over time due to wear and tear. Common causes include:
- Age-related disc degeneration
- Repetitive bending, lifting, or twisting
- Improper lifting techniques
- A traumatic injury, such as a fall or car accident
- Poor posture or prolonged sitting
- Genetics, which may make some people more prone to disc problems
As we age, our discs naturally lose water content and flexibility. This makes them more likely to tear or rupture under pressure.
Signs and Symptoms to Watch For
Symptoms of a herniated disc vary depending on the location and severity of the disc rupture. Some people may not feel any pain at all, while others may experience significant discomfort that affects daily life.
Common symptoms include:
- Localized pain in the neck, upper back, or lower back
- Radiating pain down the arm (from a cervical herniation) or leg (from a lumbar herniation)
- Tingling or numbness in the shoulder, arm, hand, buttock, leg, or foot
- Muscle weakness in the limbs, making it difficult to lift objects or maintain balance
- Pain that worsens with certain movements, such as bending or sitting
- Relief when lying flat or changing positions
In more serious cases, a herniated disc may compress spinal nerves enough to cause problems with bladder or bowel control. This is a medical emergency and requires immediate attention.
Diagnosing a Herniated Disc
If you’re experiencing persistent back or neck pain, especially with radiating symptoms, it’s important to be evaluated by a spine specialist. At Florida Surgery Consultants, we start with a physical exam and review of your medical history to identify possible disc involvement.
To confirm the diagnosis and rule out other conditions, we may recommend imaging tests such as:
- MRI scans, which show the disc material and nearby nerve roots
- CT scans to provide cross-sectional views of the spine
- X-rays, which help detect other spinal changes, such as bone spurs or alignment issues
- Nerve studies if you have numbness or weakness
These tests help determine the location of the herniated disc and the severity of nerve involvement, which is essential for creating an effective treatment plan.
Conservative Care: First-Line Treatments
The majority of herniated disc cases do not require surgery. Many people find relief through conservative, non-invasive treatments. The goal is to reduce pain, restore function, and help the disc heal naturally over time.
Conservative treatment options may include:
- Physical therapy: Guided exercises to strengthen the muscles that support your spine, improve posture, and reduce pressure on the affected disc.
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation and pain. In some cases, muscle relaxants or short-term corticosteroids may be used.
- Activity modification: Avoiding movements that trigger symptoms and gradually returning to normal activity as pain improves.
- Hot and cold therapy: Applying ice to reduce inflammation and heat to relieve muscle tension.
- Epidural steroid injections: Anti-inflammatory medication is delivered directly to the affected nerve root to reduce swelling and pain. These injections can provide temporary relief to support physical therapy and avoid surgery.
At Florida Surgery Consultants, we often combine several of these approaches, alongside your physical therapist and chiropractor, to support healing and reduce the need for surgery. Most patients start to see improvement within a few weeks.
When Is Surgery Needed?
While many people improve with conservative treatment, some may continue to experience pain, weakness, or functional limitations. If your symptoms persist beyond six to twelve weeks, or if your condition worsens, surgical intervention may be considered.
Surgery may be recommended if:
- You have severe pain that doesn’t respond to other treatments
- There’s significant muscle weakness affecting mobility or daily function
- Imaging shows nerve compression that’s likely to cause long-term damage
- You’ve experienced loss of bladder or bowel control (a rare but serious sign of spinal cord compression)
The goal of surgery is to remove the portion of the disc that is pressing on the nerve while preserving as much of the disc as possible.
Surgical Options for Herniated Discs
Florida Surgery Consultants specializes in minimally invasive spine surgery. These techniques allow for smaller incisions, less tissue damage, shorter recovery times, and reduced risk of complications.
Common procedures include:
- Microdiscectomy: A minimally invasive surgery that removes the herniated portion of the disc through a small incision.
- Laminectomy: Removal of a portion of bone (the lamina) to relieve pressure on the spinal cord or nerves.
- Spinal fusion: In cases of severe instability or multiple disc herniations, spinal fusion may be used to join two or more vertebrae. This is typically reserved for cases where other treatments have been tried and have been ineffective in pain relief.
- Percutaneous laser disc decompression: A laser technique that reduces pressure in the disc to alleviate symptoms without open surgery. More discussion with your provider is necessary to determine if this is an appropriate option.
Your surgeon will help you understand the risks and benefits of each option and recommend the approach best suited to your condition and lifestyle.
Life After Treatment
Recovery from a herniated disc depends on the severity of the condition and the treatment used. Most people who undergo conservative care can return to regular activity within a few weeks. Those who have surgery often experience significant symptom relief within one to three months.
Post-treatment goals include:
- Regaining strength and mobility
- Preventing future injuries
- Resuming work, exercise, and daily activities with confidence
- Continuing physical therapy, if recommended
It’s important to follow your provider’s instructions and attend follow-up appointments to monitor your progress.
When to Seek Help
If you’ve been living with back or neck pain, or if symptoms are interfering with your ability to move, sleep, or work, don’t wait for things to get worse. Herniated discs are treatable, and many patients see major improvements with the right care.
Early diagnosis and intervention can prevent long-term nerve damage and improve your quality of life.
Next Steps
Herniated discs can be painful, but they don’t have to control your life. With expert evaluation and a personalized treatment plan, it’s possible to reduce your symptoms, protect your spine, and return to the activities you enjoy.
Schedule a consultation with Florida Surgery Consultants to explore your options. Our team offers advanced diagnostics, conservative therapies, and minimally invasive surgical care tailored to your needs.