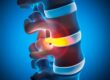
Function of Discs in Back
The discs in your back serve three very important purposes. First, they help absorb shock on the spine. Second, they function in a manner comparable to ligaments, holding the vertebrae of the spine in place. And third, they are cartilaginous joints that improve flexibility and mobility. When you discover a problem with one of your discs, such as a bulging disc, all three of these functions can be affected, resulting in acute or chronic pain, numbness, spasms, limited mobility, and a host of other symptoms. When it comes to bulging discs, effective treatment comes in many forms. For some, relief can be found by pairing physical therapy with medication. For severe cases, a surgical option may be the only path to recovery.
What Are Bulging Discs?
A bulging disc can occur in just about anyone for any number of reasons. This is a common spinal injury that affects everyone differently, and this will be reflected in your diagnosis if you decide to seek help. You have 23 discs in your spine, and any one of them can become damaged. To understand what happens when a disc bulges, you must first understand the two key components of an intervertebral disc: the external annulus fibrosus and the internal nucleus pulposus.
The external annulus fibrosus is the hard outer shell of the disc. Its layers of fibrocartilage are dense and rigid, giving you the stability you need to live an active lifestyle. This portion of the disc significantly differs from the other important element, the internal nucleus pulposus. This soft, gel-like substance is contained within the annulus, where it provides shock absorption and promotes flexibility. When a disc bulges, one of three things can happen:
- The annulus is the first portion of the disc to be affected, becoming warped over time. If this disfiguration causes the annulus to make contact with a spinal nerve, it can cause pain, stiffness, or muscle spasms. There is also a chance that this type of bulging disc will have no symptoms.
- As the condition progresses, the bulge’s impact on the nerves will continue to increase. If the bulge is asymmetrical, symptoms can be more severe.
- Once the nucleus of the disc has ruptured and “bulged” through the annulus, the bulging disc has officially progressed to a condition known as a herniated disc.
- The nature and severity of the injury will also affect which symptoms occur, which means individualized treatment is an essential element for a successful recovery.
What is the difference between a bulging disc and a herniated disc?
Although often used interchangeably, bulging discs and herniated discs are not the same. A herniated disc is a more severe form of a bulging disc. Whereas a bulging disk affects between a quarter and half of the disk’s outer layer, a herniated disc is the result of a much deeper wound. When the annulus is damaged to the point that the gel-like nucleus begins to protrude out, a bulging disc has officially progressed to a herniated disc. Individuals with a herniated disc are more prone to pain than those with a bulging disc. Typically, the more the disc begins to bulge, the more likely it is to irritate a nerve, resulting in more intense pain.
How Are Bulging Discs Diagnosed?
There are several ways to diagnose a bulging disk. The most simple way is with a physical exam, although a neurological exam can be used as well. A neurological exam tests your reflexes, muscle strength, walking ability, and ability to feel various sensations. Your medical history is also an important component of this initial diagnosis. If something seems off with your spinal health, your medical provider will likely suggest that you undergo some form of imaging test to confirm the problem. Several imaging tests are effective for diagnosing bulging discs, including X-rays, CT scans, MRIs, and myelograms. Additionally, a nerve conduction study and electromyography can be used to gain insight on any damage along your spine. These nerve tests deal with the interplay of electrical impulses and your nerve tissue.
Bulging Disc Signs To Be Aware Of
Bulging discs are a common condition; in fact, they’re a natural part of the aging process. Which explains why some people never experience pain from their bulging discs, while others can barely move when their pain is flaring up. When you do experience pain, it means your disc has made contact with a nerve. It also means it’s time to contact your local neurosurgeon or orthopedic specialist. Some other signs to be on the lookout for include:
- Sharp pain in your legs or buttocks
- Radiating pain in your neck or extremities
- Numbness or tingling
- Weakness
If you experience any of these symptoms, don’t hesitate to call a spine specialist for treatment. Depending on the severity of your condition, your bulging disc may be treatable with physical therapy, non-steroidal anti-inflammatory drugs, steroid injections, or surgery.
What Are The Surgical Options For a Bulging Disc?
When conservative treatments fail to provide you with relief from your pain, it’s time to consider a surgical option. Month after month of daily pain can wear on anyone. You deserve relief, and Florida Surgery Consultants are standing by to conduct the surgery that is right for your age, medical history, and level of health. There are several highly effective surgeries that can be employed to correct a bulging disc, such as:
Artificial Disc Replacement: replaces the damaged disc with a polyethylene or metal substitute.
Dekompressor Discectomy: a minimally invasive procedure that gives your surgeon access to the affected disc, which is then removed to alleviate pressure on the nerve.
Interbody Fusion: oftentimes utilized for those suffering from degenerative disc disease. This surgery replaces the damaged disc with bone grafts and metal. These pieces are then fused to the vertebrae.
Selective Endoscopic Discectomy: a small tube with a light and camera are used to view the damaged disc. This same tool can be used to remove the bulging cartilage and cauterize the area.
Best of all, many of these surgeries do not require an extended hospitalization. In fact, most minimally invasive surgeries allow the patient to return home the day of surgery. Following your surgery, your doctor will recommend a strict diet, exercise, and pain management regimen. You will want to follow these instructions closely to accelerate your recovery and get back to your regular lifestyle. The decision is in your hands. Contact the professionals at Florida Surgery Consultants for assistance today, and enjoy a pain-free life tomorrow.
Bulging Disc Facts
- Anatomy and Basics: Intervertebral discs are fibrocartilaginous cushions situated between the vertebrae of the spinal column. They consist of a soft, gel-like center called the nucleus pulposus and a tougher, fibrous outer layer called the annulus fibrosus.
- Definition: A bulging disc occurs when the disc’s outer layer (annulus fibrosus) weakens and uniformly protrudes out of its normal space but doesn’t rupture. This is different from a herniated disc, where the soft inner material (nucleus pulposus) breaks through the outer layer.
- Causes: Common causes include aging (natural degenerative processes), wear and tear, injury, strain, genetic factors, or a combination thereof.
- Symptoms: Not all bulging discs produce symptoms. When they do, it’s typically because the bulging area is pressing on a nerve. Symptoms can include localized pain, tingling, numbness, or weakness in the areas of the body that the affected nerve serves.
- Diagnosis: Imaging studies such as MRI (Magnetic Resonance Imaging) or CT (Computed Tomography) scans are commonly used to diagnose bulging discs.
- Treatment: Many bulging discs can be managed non-surgically with a combination of rest, physical therapy, anti-inflammatory medications, pain-relieving medications, or epidural steroid injections. Only in severe or non-responsive cases is surgery considered.
- Prevention: While some factors (like aging and genetics) cannot be controlled, maintaining a healthy weight, practicing good posture, avoiding repetitive strain or injury, and strengthening core muscles can all help reduce the risk of developing a bulging disc.
- Location Matters: Bulging discs are most common in the lumbar region (lower back) due to the weight and motion it supports. They can also occur in the cervical (neck) and thoracic (mid-back) regions, although less frequently.
- Natural Degeneration: As people age, discs naturally lose hydration and become less flexible, increasing the chances of disc bulging.
- Not Always Permanent: With the right treatment and care, many bulging discs can heal or become asymptomatic over time.